Your doctor handed you a report with 20 numbers on it and told you everything looks fine. But one value is flagged in red. What does it mean?
Feeling Lost? You are not alone. The Complete Blood Count (CBC) is one of the most commonly ordered blood tests in the world. Yet, most people have no idea what it is actually measuring.
In this article, we will walk through each part of a CBC blood test report in plain language. By the end, you will understand what normal and abnormal results can mean. More importantly, you will know exactly what your doctor is looking for — without the medical jargon.
What does a Complete Blood Count (CBC blood test) Measure?
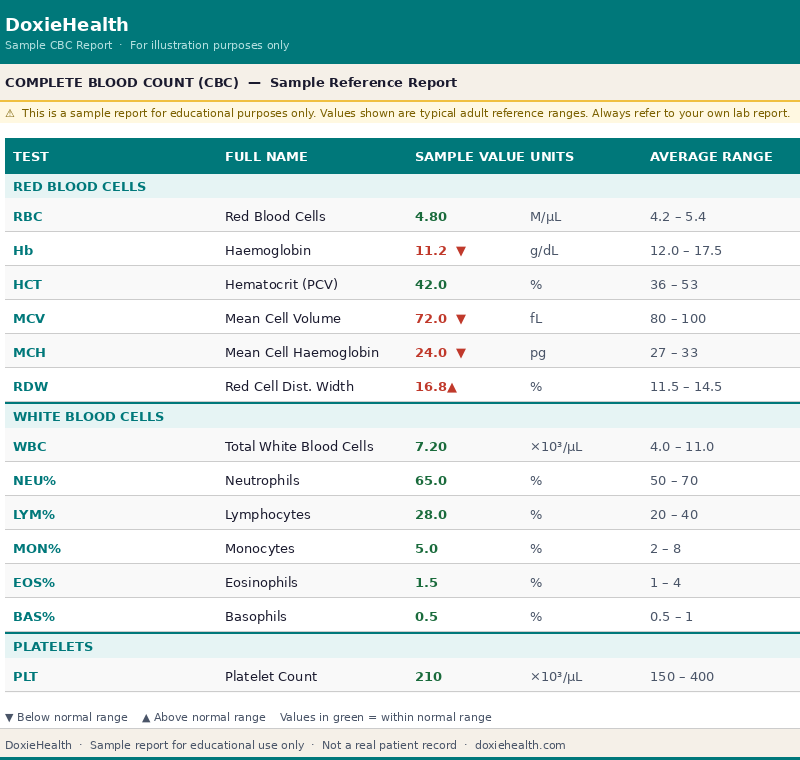
A CBC blood test measures three main types of cells circulating in your blood: red blood cells (RBC), white blood cells (WBC), and platelets.
Together, these cells give your doctor a clear picture of some of the body’s most essential systems.
In addition, the test does more than count cells. It also measures haemoglobin, hematocrit, and red cell indices.
These markers help show the quality and characteristics of your red blood cells.
In simple terms, you can think of a CBC as a snapshot of what is happening inside your blood at a given moment.
Because of this, it is often the first test doctors order when they suspect something may be wrong.
As a result, a single CBC blood test can help detect a wide range of conditions, from nutritional deficiencies and infections to the early signs of more serious illnesses.
Quick Reference: Normal CBC blood test Ranges
General adult reference ranges. Your lab may show slightly different values.
| Marker | What It Measures | Male | Female |
|---|---|---|---|
| RBC | Oxygen-carrying cells | 4.5–5.5 M/µL | 4.0–5.0 M/µL |
| Hemoglobin | Oxygen-carrying protein in RBCs | 13.5–17.5 g/dL | 12.0–15.5 g/dL |
| Hematocrit | Haemoglobin content per red cell | 41–53% | 36–46% |
| WBC (Total) | Total immune defence cells | 4,000–11,000/µL | 4,000–11,000/µL |
| Platelets | Clotting cells | 1.5–4.0 × 10⁵/µL | 1.5–4.0 × 10⁵/µL |
| MCV | Average size of red blood cells | 80–100 fL | 80–100 fL |
| MCH | Hemoglobin content per red cell | 27–33 pg | 27–33 pg |
| RDW | Variation in red cell size | 11.5–14.5% | 11.5–14.5% |
WBC differential breakdown (neutrophils, lymphocytes, eosinophils, monocytes, basophils) is explained in detail in Section 4.
Red Blood Cells (RBC)
Red blood cells carry oxygen from your lungs to every tissue in your body. As a result, they play a crucial role in keeping your organs functioning properly.
When the number of red blood cells drops, your tissues receive less oxygen. Over time, this can make your body feel tired and strained.
When RBC is Low
Common symptoms may include:
- Persistent fatigue or weakness
- Shortness of breath, even with light activity
- Pale or yellowish skin
- Dizziness or difficulty concentrating
Therefore, the first question your doctor will ask is: Why is your body not making enough red blood cells?
In many cases, the cause is a nutritional deficiency, such as low iron, vitamin B12, or folate. In addition, certain chronic illnesses — including kidney disease or inflammatory bowel disease — can interfere with the body’s ability to produce healthy red blood cells.
Less commonly, the problem originates in the bone marrow, the spongy tissue inside your bones where all blood cells are produced. If the bone marrow becomes damaged or suppressed, it may fail to produce enough red blood cells.
Importantly, these situations often affect white blood cells and platelets as well. For this reason, doctors pay close attention when multiple CBC values are low simultaneously.
When RBC is High
Elevated RBC levels are less common. However, they may occur in situations where the body is trying to compensate for lower oxygen levels.
For example, dehydration, smoking, or living at a high altitude can push the body to produce more red blood cells in order to carry additional oxygen.
Haemoglobin (Hb)
Haemoglobin is the oxygen-carrying protein inside red blood cells. In many ways, it is the most important number in a CBC report.
Because it most directly reflects your blood’s ability to deliver oxygen throughout the body.
Signs of Low Haemoglobin
- Persistent tiredness that does not improve with rest
- Dizziness or light-headedness
- Frequent headaches
- Getting breathless doing things that never used to tire you
Common causes include:
- Iron deficiency — the most frequent cause worldwide
- Vitamin B12 or folate deficiency — affects how red blood cells are produced
- Chronic blood loss — heavy periods, gut bleeding, etc. This list is not exhaustive — any source of ongoing blood loss can contribute.
- Chronic diseases — kidney disease, autoimmune conditions, cancer, etc.
Therefore, doctors rarely interpret haemoglobin in isolation. Instead, they read it alongside other CBC markers — particularly MCV and RDW — to identify the type and underlying cause of anaemia, rather than simply confirming that anaemia is present.
Hematocrit (HCT)
Hematocrit tells you what percentage of your blood is made up of red blood cells. Because of this, it is closely linked to haemoglobin and usually moves in the same direction.
When hematocrit levels are low, it almost always confirms the presence of anaemia.
On the other hand, a high hematocrit is most commonly caused by dehydration.
To understand why, it helps to think about how blood is structured. Your blood is made up of red blood cells and a watery liquid called plasma.
When you become dehydrated, the plasma portion shrinks. As a result, red blood cells make up a larger percentage of the remaining blood, even though the actual number of red cells has not increased.
In simple terms, it is like a glass of orange juice becoming more concentrated as some of the water evaporates.
White Blood Cells (WBC)
White blood cells form the frontline of your immune system. Whenever the body senses a threat — such as an infection, inflammation, or tissue injury — it quickly mobilises these cells to respond.
For this reason, the WBC count is often one of the earliest warning signs that something is triggering your immune system in a CBC blood test report.
High WBC Count
An elevated WBC count usually indicates that the immune system is actively responding to something in the body.
- Bacterial infections — often a significant rise
- Inflammation or physical stress — inflammation is the body’s internal alarm response: when tissues are irritated or injured (even by things like surgery, intense exercise, or autoimmune flare-ups), white cells are sent in, which temporarily raises the count.
- Certain medications or steroid use.
- Rarely, blood disorders such as leukaemia.
Low WBC Count
On the other hand, a low WBC count can occur with:
- Viral infections — the WBC can temporarily dip
- Certain medications, such as chemotherapy agents
- Bone marrow suppression (e.g., from cancer treatment, certain autoimmune conditions) — this is less common but important to evaluate.
WBC Differential — What Each Type Tells Your Doctor
Beyond the total WBC count, doctors also examine the WBC differential, which shows the proportion of each type of white blood cell.
This breakdown shows what the immune system is responding to. Each cell type has a specific role:
| Neutrophils (50–70%) — First responders. High neutrophils usually mean physical stress or bacterial infection. Lymphocytes (20–40%) — The memory cells of your immune system. High lymphocytes are common in viral infections (flu, COVID-19, glandular fever). Monocytes (2–8%) — Cleanup crew. They rise during chronic infection or autoimmune conditions. Eosinophils (1–4%) — Rise during allergies, asthma, or parasitic infections. Basophils (0.5–1%) — The rarest type. Involved in allergic and inflammatory responses. In summary, the total WBC count provides only part of the story. The differential is what allows doctors to understand the underlying cause of the immune response. |
A Note on Total vs Absolute WBC Count
Your CBC report may show two types of WBC measurements.
- Total leukocyte count refers to the overall number of white blood cells present in your blood.
- Absolute counts for each cell type — such as absolute neutrophils or absolute lymphocytes — show the exact number of that specific cell in the blood, rather than just its percentage.
Both measurements are useful. However, doctors often rely more on absolute counts when evaluating specific conditions because percentages alone can be misleading when the total WBC count is unusually high or low.
Platelets
Platelets are tiny, disc-shaped cells that rush to the site of any injury to form a clot and stop bleeding.
Without enough platelets, even a small cut can bleed longer than normal. In simple terms, they are your body’s emergency repair crew.
Low Platelet Count (Thrombocytopenia)
When platelet levels drop too low, the blood cannot clot efficiently. As a result, people may notice symptoms such as:
- Easy bruising
- Nosebleeds or bleeding gums
- Prolonged bleeding from minor cuts
- Tiny red or purple dots on the skin (petechiae)
Low platelet counts can occur due to viral infections, certain medications, immune disorders, or bone marrow problems.
In many cases, the drop is temporary, but significantly low levels require medical evaluation.
High Platelet Count (Thrombocytosis)
On the other hand, an elevated platelet count most often occurs as a reactive response. This means the body is responding to another condition, such as infection, inflammation, or surgery.
This type of increase is called reactive thrombocytosis, and it usually resolves once the underlying condition improves. For this reason, it is rarely a cause for concern on its own.
Less commonly, high platelets may point to a bone marrow disorder called essential thrombocythaemia. Here, the bone marrow produces excess platelets with no external trigger.
Unlike reactive thrombocytosis, this condition requires specialist evaluation and monitoring.
Red Cell Indices — MCV, MCH & RDW
These three markers go beyond simply counting red blood cells. Instead, they describe the size, haemoglobin content, and uniformity of red blood cells.
Together, they help doctors identify the underlying cause of anaemia, rather than simply confirming that anaemia is present.
| Marker | What It Measures | Low Value | High Value | Special Note |
| MCV | Average size of red blood cells | Small cells · Iron deficiency anaemia · Thalassaemia trait | Large Cells · Vitamin B12/Folate Deficiency · Hypothyroidism | Key for classifying anaemia type |
MCH | Haemoglobin content per red cell | Pale, poorly filled cells (hypochromic) · Iron deficiency anaemia | Oversized, overfilled cells · B12/folate deficiency | Usually moves in parallel with MCV |
| RDW | Variation in red cell size | Rare, uniformly sized cells | Mixed cell sizes · Iron, B12/folate deficiency · Post-chemotherapy | Can rise before haemoglobin drops |
MCV = Mean Corpuscular Volume · MCH = Mean Corpuscular Haemoglobin · RDW = Red Cell Distribution Width. Normal ranges: MCV 80–100 fL · MCH 27–33 pg · RDW 11.5–14.5%
MCH typically moves in parallel with MCV — larger cells tend to contain more haemoglobin.
Because haemoglobin is responsible for carrying oxygen, this marker helps assess how well each cell performs its job
RDW is a sensitive early marker. It may provide an early clue that the body is struggling to produce healthy, uniform red blood cells.
| 👩⚕️ Doctor’s Note A single slightly abnormal CBC value is not a diagnosis. Doctors always interpret results in clinical context — together with your symptoms, medical history, and other test results. Numbers alone do not tell the whole story. Context does. |
When Should You Be Concerned?
Certain patterns in a CBC blood test report are worth discussing with your doctor, especially if they appear alongside symptoms:
- Low Hb + Low MCV + High RDW→ Likely iron deficiency. Common, treatable.
- Low Hb + High MCV→ Consider B12 or folate deficiency. Check diet and absorption.
- High WBC→ Possible infection or inflammation. Look at the differential for more details.
- Very Low WBC→ Worth investigating — especially if on medications or feeling unwell.
- Low Platelets→ Easy bruising or bleeding? Report to your doctor promptly.
Always bring your actual laboratory reports to your doctor. Numbers with context — not numbers in isolation — are what matter.
The Takeaway
The Complete Blood Count is a deceptively simple test. From a single blood sample, it can reveal signs of anaemia, immune activity, nutritional deficiencies, and bone marrow function — all at once. In short, it packs a remarkable amount of information into one report.
Understanding your CBC blood test report does not mean diagnosing yourself. Instead, it means arriving at your doctor’s appointment informed, calm, and ready to ask the right questions.
That is exactly what we aim to help you do at DoxieHealth.
Questions to Ask Your Doctor
Reading your CBC blood test report before your appointment is only half the job. Arriving with the right questions is the other half. Here are four questions worth raising:
- “My haemoglobin is low — what is the next step to find the cause?” Low Hb has several possible causes, and the treatment depends entirely on which one it is. This question prompts your doctor to explain their reasoning rather than just hand you a prescription.
- “My WBC is elevated — should I repeat this test, or do we investigate now?” A single elevated WBC can be a temporary response to infection or stress. This question helps you understand whether your doctor wants to monitor or act immediately.
- “My RDW is high, but my haemoglobin is still normal — does that need attention?” RDW can rise early, before anaemia develops. This question shows your doctor you have read your report carefully, and surfaces a finding that might otherwise be overlooked.
- “Are there any values here that need a follow-up test, or is this result complete on its own?” A CBC is often the starting point, not the full picture. This open-ended question invites your doctor to flag anything that needs further investigation — iron studies, B12 levels, thyroid panel, and so on.
References & Further Reading
This article is grounded in established clinical guidelines and peer-reviewed literature. Key sources include:
- World Health Organization (WHO). Haemoglobin concentrations for the diagnosis of anaemia and assessment of severity. Geneva: WHO, 2011. Available at: Haemoglobin concentrations for the diagnosis of anaemia and assessment of severity
- NHS (National Health Service, UK). Full blood count (FBC) — what the results mean. Available at: Blood tests – NHS
- Mayo Clinic. Complete blood count (CBC) — what you can expect. Rochester: Mayo Foundation for Medical Education and Research. Available at: Complete blood count (CBC) – Mayo Clinic
- Buttarello M, Plebani M. Automated blood cell counts: state of the art. American Journal of Clinical Pathology. 2008;130(1):104–116.Available at: https://pubmed.ncbi.nlm.nih.gov/18550479/
- MedlinePlus (U.S. National Library of Medicine). Complete blood count (CBC) — what the results mean. Available at: Complete Blood Count (CBC) — MedlinePlus
Medical Disclaimer: This article is for educational purposes only and does not constitute medical advice, diagnosis, or treatment. Always consult a qualified healthcare professional for guidance about your specific health situation.
Leave a Reply