You’re holding your blood report, your eyes drawn to three numbers: HbA1c, Fasting Blood Sugar, and Post-Prandial Blood Sugar, and especially the HbA1c normal range. Something about them made you pause.
That pause is important.
Because tucked inside your report is a gentle but powerful insight into your health. And it all begins with understanding your HbA1c normal range — the number that tells the honest story of your blood sugar over the past three months.
Once you understand it, everything else in the report starts to make sense. You’ll know what your numbers truly mean, why HbA1c matters most, and what your next step should be.
The Organ You Never Notice — Until Blood Sugar Changes: The Pancreas
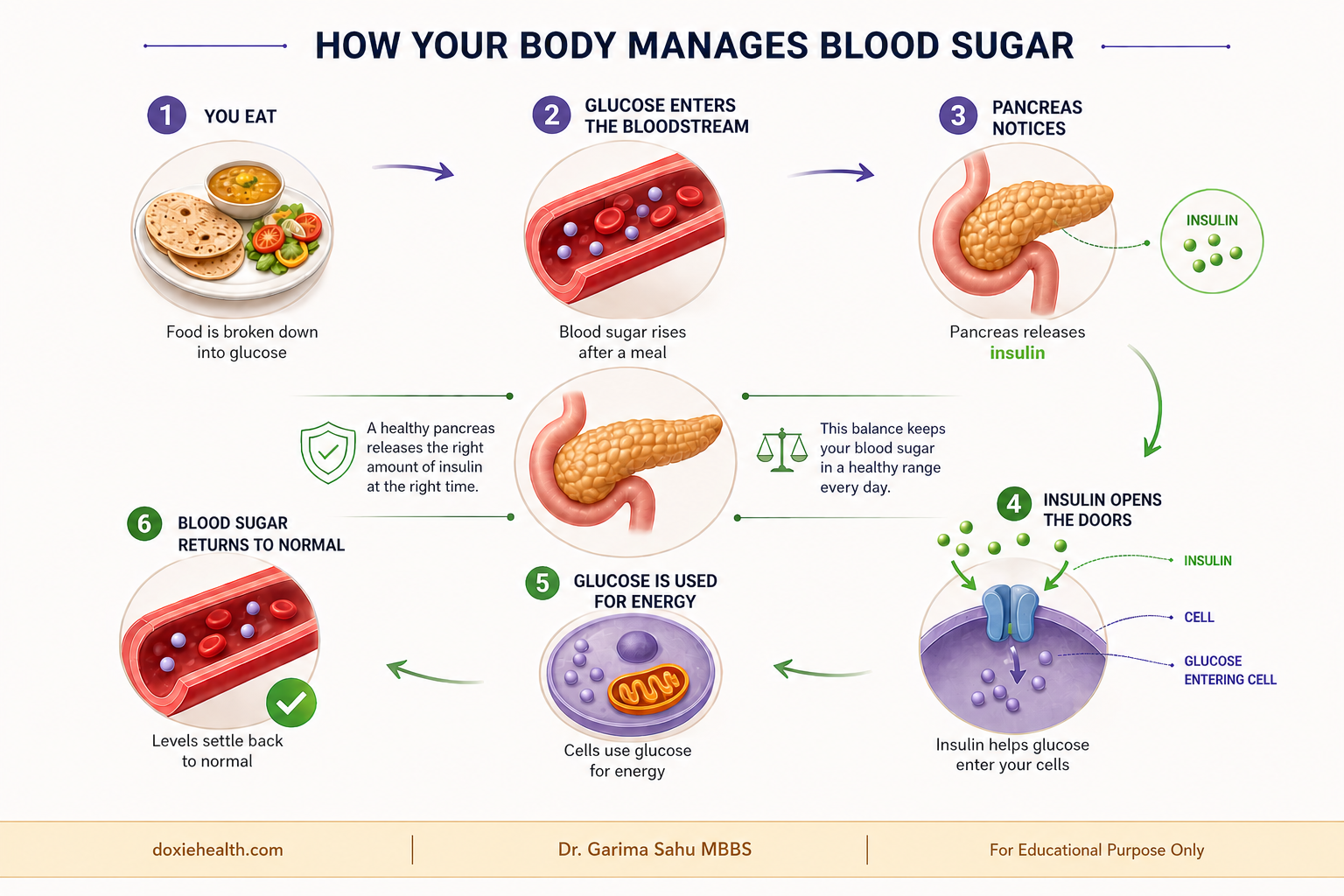
Your body has a silent guardian, a master regulator of blood sugar. Meet your pancreas.
Most of us imagine blood sugar as something that only spikes with sweets and sodas. The truth is far more elegant and constant.
Every morsel you eat, whether it’s warm roti, comforting dal, or a quick banana, is broken down by your digestive system into glucose (Sugar). That glucose slips into your bloodstream, turning your meal into fuel for life itself.
The moment those glucose levels begin to rise, your pancreas stirs.
Tucked quietly behind your stomach, this unassuming organ senses the change with exquisite precision. It releases insulin, a hormone that acts like a gentle key – unlocking the doors of your cells so glucose can enter and be burned for energy.
Within a couple of hours, the surge settles. Blood sugar rises modestly after eating, then returns to its calm baseline. You feel nothing dramatic. You’re not meant to. That smooth rhythm is health at work.
But when the pancreas grows weary—when it cannot produce enough insulin, or when your cells slowly stop listening—the return journey falters. Glucose lingers in the blood like an uninvited guest. The delicate balance begins to shift.
And that is exactly what these three tests are quietly trying to tell you.
Your Quick Reference — All Three Tests at a Glance
Before we go deeper, here’s the full picture. Find your numbers and then read on – because knowing the range is only the beginning.
| Test | Normal | Prediabetes | Diabetes |
| HbA1c | Below 5.7% | 5.7% – 6.4% | 6.5% or above |
| Fasting Blood Sugar (FBS) | Below 100 mg/dL | 100 – 125 mg/dL | 126 mg/dL or above |
| Post-Prandial Sugar (PPBS) | Below 140 mg/dL | 140 – 199 mg/dL | 200 mg/dL or above |
Source: American Diabetes Association Standards of Care, 2024. WHO criteria: prediabetes from HbA1c 6.0%, diabetes at 6.5%.
HbA1c Normal Range: The Test That Sees the Whole Picture
Most blood sugar tests (FBS and PPBS) are snapshots — a single frame from a very long film.
A stressful morning, a restless night, or a late dinner can quietly shape that one reading. The number is truthful, yes — but it belongs only to that moment.
And moments can be deceiving. One careful meal or a day of extra discipline can make the result look reassuring, even if the bigger story has been unfolding very differently.
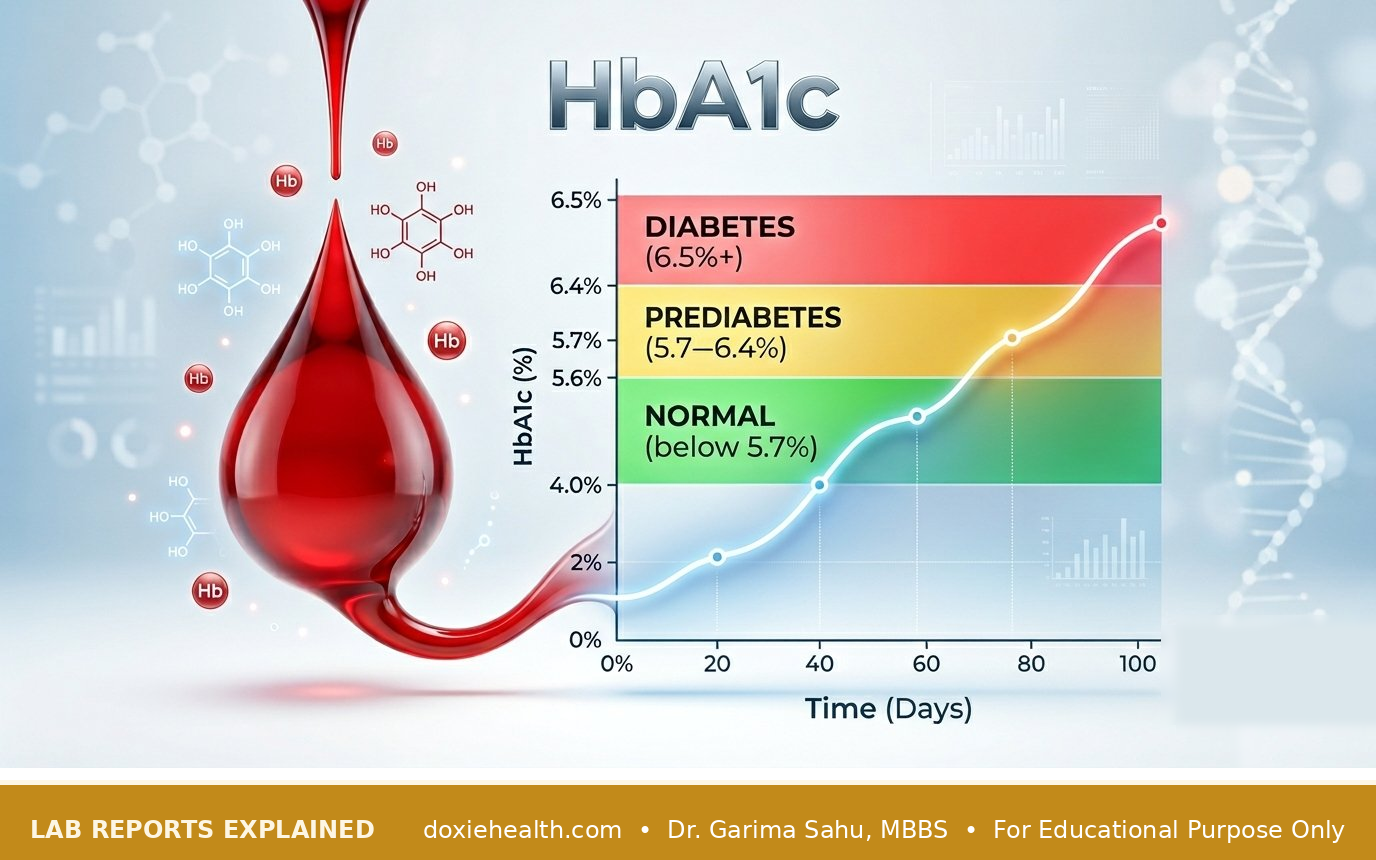
HbA1c doesn’t work that way. Think of HbA1c as your blood sugar’s long-term diary.
Every day, tiny sugar molecules drift through your bloodstream and quietly latch onto haemoglobin — the protein living inside your red blood cells in your blood. The more sugar that circulates, the more of these little attachments form.
| Now here’s the beautiful part: Red blood cells stay with you for about three months. They witness your best days, your indulgent days, your disciplined days, and everything in between. So when we measure HbA1c, we’re not looking at a single moment in time. We’re reading a three-month story — a gentle, honest summary of how your blood sugar has truly behaved. |
One wedding dinner won’t move it. Three months of consistently high sugar will.
This is why HbA1c is the gold standard. While FBS and PPBS can shift with stress, sleep, and what you ate the night before, HbA1c is far more stable and far more reliable as a long-term indicator.
Many people feel reassured when their fasting or post-meal sugar looks normal, and that reassurance can be misleading. HbA1c is the number that tells you what’s really been happening.
| HbA1c | What It Means |
| Below 5.7% | Normal |
| 5.7% – 6.4% | Prediabetes |
| 6.5% or above | Diabetes |
| How often should you test HbA1c? -No risk factors, normal result → once a year -Prediabetes range → every 3 to 6 months -Diagnosed diabetes → every quarter (every 3 months) |
A Note That Some Indian Patients May Need to Read
In most cases, HbA1c is straightforward and reliable. But occasionally — in a small number of people — the result can be misleading.
| If you have iron deficiency anaemia or carry the thalassaemia trait, there is a chance your HbA1c may not accurately reflect your true blood sugar. These conditions affect red blood cells in ways that can subtly skew the reading — sometimes higher, sometimes lower than the reality. |
This doesn’t mean your result is wrong. It means if your report has also flagged low haemoglobin or abnormal red cell indices, bring both reports to your doctor together. In those cases, Fasting Blood Sugar and Post-Prandial Sugar become the more dependable guides.
Not sure what your CBC report is telling you? → CBC Blood Test: What Your Results Really Mean
Fasting Blood Sugar: Your Body’s Overnight Report Card
| Fasting Blood Sugar (FBS) is measured after at least 8 hours without food — almost always first thing in the morning. |
By that point, your last meal has been processed, cleared, and forgotten. What you’re seeing now is your body’s resting baseline — how much sugar it holds onto even when it has nothing new to work with.
In a healthy body, this number stays low and stable overnight. When it starts creeping up, it’s a quiet signal that blood sugar regulation is loosening.
| FBS Level | What It Means |
| Below 100 mg/dL | Normal |
| 100 – 125 mg/dL | Prediabetes (Impaired Fasting Glucose) |
| 126 mg/dL or above | Diabetes |
A single elevated reading doesn’t automatically mean something is wrong — a stressful week, poor sleep, or being unwell can nudge this number up temporarily.
Your doctor will confirm with a repeat test before drawing any conclusions. But if it’s consistently above 100? Your body is sending a signal. Don’t ignore it.
| How often should you test FBS? – Low risk, normal result → once in two years or once a year is sufficient – Risk factors present (family history, overweight, sedentary lifestyle) → annually – Prediabetes → as directed by your doctor, often alongside your HbA1c – Diagnosed with diabetes → every quarter alongside HbA1c, or as your doctor advises |
Post-Prandial Sugar: The Test That Catches What FBS Misses
| PPBS is measured exactly two hours after a full meal — and in that short window, it reveals what fasting sugar never can. |
The moment you eat, your pancreas springs into action. It releases insulin into the bloodstream, sending a quiet message to every cell: open up, let the sugar in.
When this conversation flows smoothly, blood sugar rises gently after a meal, peaks within about an hour, and then slips back to normal by the two-hour mark.
You don’t feel the work being done. Your body handles it with quiet efficiency.
But over time, the conversation begins to change. Cells start becoming resistant to insulin’s gentle knock. The signal is sent, yet the doors don’t open as easily. Sugar lingers in the bloodstream, unsure where to go. The rise becomes higher. The fall becomes slower.
| And this is where PPBS becomes a quiet detective — often spotting the earliest signs of insulin resistance years before fasting sugar ever hints that something has begun to shift. |
| PPBS (2-hour) | What It Means |
| Below 140 mg/dL | Normal |
| 140 – 199 mg/dL | Prediabetes (Impaired Glucose Tolerance) |
| 200 mg/dL or above | Diabetes |
For context: a typical Indian meal — rice, two rotis, dal, sabzi — carries a substantial carbohydrate load. Some rise in post-meal sugar is completely normal. But if your body is regularly struggling to bring it back below 140 mg/dL by the two-hour mark, that’s a pattern worth taking seriously.
| How often should you test PPBS? – Routine screening → usually alongside FBS, as directed by your doctor – Monitoring prediabetes or diabetes → based on your doctor’s guidance |
What High Blood Sugar Can Feel Like

This is where the story becomes quietly deceptive. Blood sugar problems rarely announce themselves with drama — not in the beginning.
Instead, they whisper.
A heaviness after meals that you’ve been calling laziness. A thirst that feels just a little more persistent than before. More trips to the bathroom, especially at night. Small cuts are taking longer to heal. That familiar afternoon fog makes focus feel harder than it once did.
Most of us explain these things away. I’m just tired. It’s the heat. I’m getting older.
Sometimes that’s true. But sometimes, your blood report is telling a different story — and now you know where to look.
If Your Numbers Are in the Prediabetes Range
Here is something most people don’t realise about prediabetes — and it changes how the whole story feels.
The Hidden Hero Inside You
At first, you would never know anything was wrong. Your fasting sugar looks almost normal. Your post-meal readings stay just within the acceptable range. Life feels ordinary. Yet beneath the surface, something profound is unfolding.
| Your pancreas, that modest, hardworking organ tucked behind your stomach, refuses to surrender without a fight. As your cells begin to lose their sensitivity to insulin, the pancreas answers the call. It pours out more and more insulin—working double shifts, then triple—desperately trying to keep your blood sugar from rising. For months, sometimes even years, it succeeds. It is a silent hero, holding the line while the rest of you go about your days unaware. |
But no organ can work overtime forever.

The Tipping Point Most People Miss
| There comes a moment—often without dramatic warning—when the overworked beta cells inside the pancreas start to tire. They slow down. They falter. And when they do, blood sugar can surge with shocking speed, crossing the threshold into diabetes far more abruptly than most people expect. What felt like a mild, manageable concern suddenly becomes something far more serious. |
This is the hidden danger most people miss.
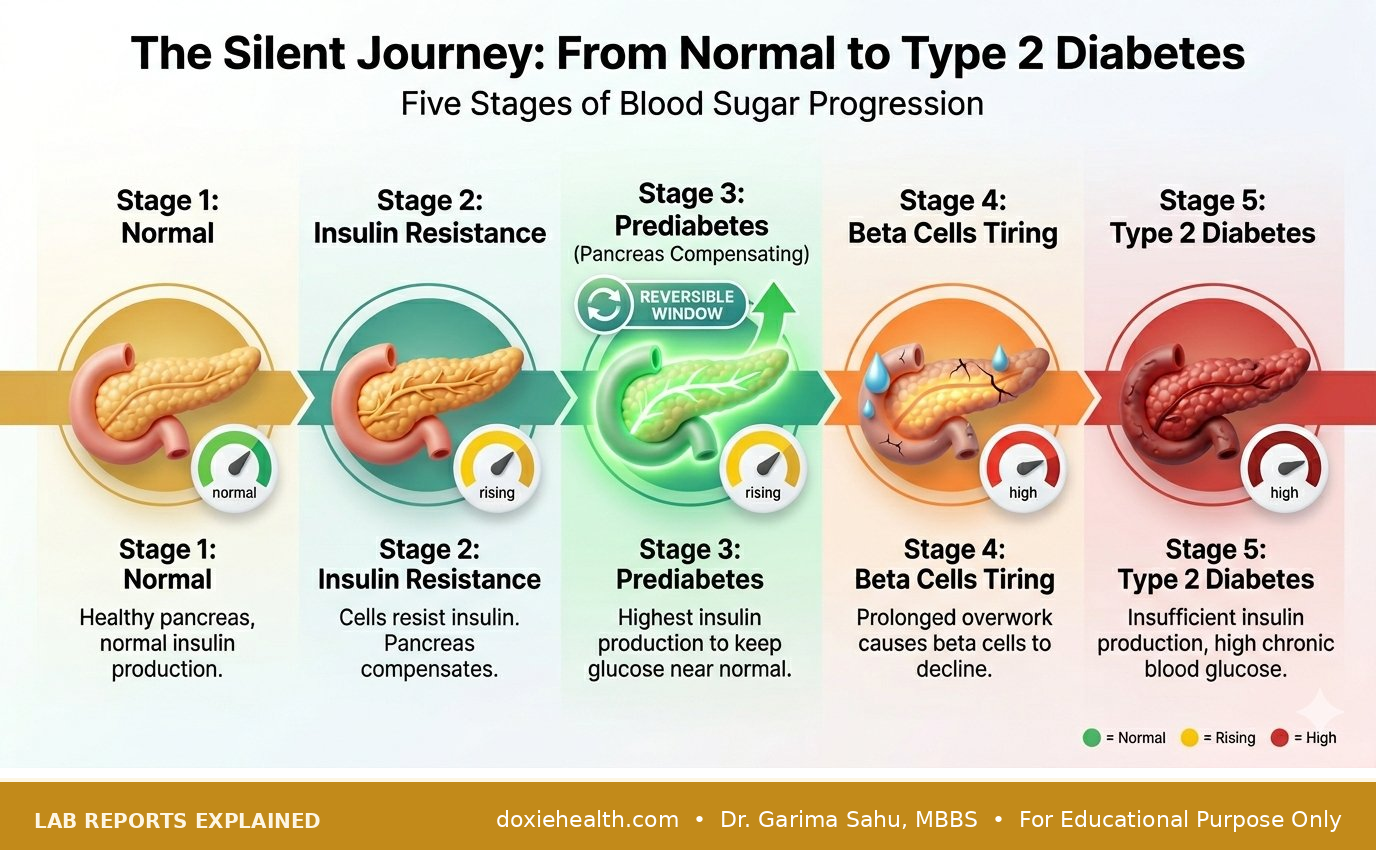
Why “Wait and Watch” Is Dangerous
This is why prediabetes is not a stage meant for waiting and watching. It is a moment meant for action. The good news—the truly hopeful news—is that the damage is still reversible for most. For many people, simple lifestyle changes are powerful enough to bring numbers back to normal.
In some cases — especially when prediabetes has lingered, or other risk factors are present — medication may also become part of the conversation. It is a conversation worth having before you leave the clinic.
Either way, the time to act is now, while the window is still open.
| Studies have shown, again and again, that people who take prediabetes seriously can slash their risk of developing full diabetes by more than half. That is a second chance at a healthy future. |
The Real Root Cause (And What You Can Do)
If you truly want to understand why this is happening to you—why your numbers are creeping up even though you haven’t changed your habits dramatically—you must look one step earlier in the chain. Before blood sugar rises, something else is quietly shifting: your cells are growing resistant to insulin itself.
That story, and what it means for you, is told here:* What Insulin Resistance Is? Signs, Causes & the Lab Markers That Reveal It.*
The more you understand, the more power you have to change the ending.
Your Report Shows a High Number — Here Is What to Do Next
A single number on a lab report can land like a sentence. It can feel like a verdict, a label, a sudden shift in the story you thought you were living.
But medicine is rarely written in a single line.
No careful doctor diagnoses diabetes from a single test. Stress, illness, poor sleep, medications, or even timing can temporarily raise blood sugar. That’s why good practice always calls for a repeat test on a different day.
One result may whisper. Two together begin to speak clearly.
If this is your first high reading, don’t panic — it’s simply time for confirmation. And even if diabetes is eventually confirmed, it is not the end of your story. It’s the beginning of a new, manageable one.
| Diabetes is serious, yes, but it is also one of the most studied and manageable chronic conditions today. Small daily choices — what you eat, how you move, consistent monitoring, and sometimes medication — can powerfully change your path ahead. |
Understanding brings control. And control brings calm.
If you’d like to understand what diabetes really means — the different types, why it happens, and what comes next — this is where your next chapter begins: Diabetes Explained: Types, Causes & What It Does to Your Body →
| 👩⚕️ Doctor’s Note |
| HbA1c, FBS, and PPBS each measure blood sugar from a different angle, and together, they tell a far more complete story than any one test alone. If your values are in the prediabetes range, don’t dismiss it and don’t panic. This is exactly the stage where your choices carry the most weight. Please bring your full report to your doctor — not just the number that worried you — and have an honest conversation about what to do next. |
When Should You Be Concerned?
- HbA1c ≥6.5% → Ask your doctor to confirm with a second test. Don’t wait for your next routine check.
- HbA1c 5.7–6.4% with elevated FBS or PPBS → Multiple markers moving in the same direction is significant. Act now.
- PPBS ≥200 mg/dL with symptoms — unusual thirst, frequent urination, unexplained fatigue, slow-healing wounds → See your doctor promptly.
- Borderline HbA1c alongside anaemia or thalassaemia in your history → Ask your doctor whether your HbA1c is reliable, or whether FBS and PPBS should be guiding the picture instead.
The Takeaway
HbA1c is your three-month average — the most honest, least manipulable reflection of where your blood sugar has really been. FBS shows how your body manages sugar at rest. PPBS reveals whether your body can bring it back down after a meal. Together, these three numbers tell a story.
You’ve just learned to read it. The next step is acting on it.
Questions to Ask Your Doctor
- My HbA1c is [X]% — do I need a second test to confirm this?
- I have anaemia — could that be affecting the accuracy of my HbA1c?
- My prediabetes has been borderline for a while — should I be on medication?
- Should I be monitoring my post-prandial sugar at home, and how?
- Which number concerns you the most — and where do we start?
References
- American Diabetes Association. Standards of Medical Care in Diabetes — 2024. Diabetes Care. 2024;47(Suppl 1). Read here →
- World Health Organization. Use of Glycated Haemoglobin (HbA1c) in the Diagnosis of Diabetes Mellitus. WHO; 2011. Read here →
- Knowler WC et al. Reduction in the incidence of type 2 diabetes with lifestyle intervention or metformin. N Engl J Med. 2002;346(6):393–403. Read here →
- Radin MS. Pitfalls in Hemoglobin A1c Measurement. Am J Med. 2014;127(1):9–15. Read here →
Medical Disclaimer: This article is for educational purposes only and does not constitute medical advice, diagnosis, or treatment. Always consult a qualified healthcare professional for guidance about your specific health situation.
WRITTEN & MEDICALLY REVIEWED BY
Dr. Garima Sahu, MBBS
Physician & Founder, DoxieHealth
This article is for educational purposes only and does not replace professional medical advice
Leave a Reply