Vitamin D deficiency is one of the most common — and most commonly missed — nutritional deficiencies in India today. Despite living in one of the sunniest countries in the world, an estimated 70-90% of urban Indians have insufficient Vitamin D levels.
Do you constantly feel tired, unmotivated, or low — even when life is going well? Do you wake up unrefreshed, struggle to focus at work, or feel a vague sense of body ache that never quite goes away? Before attributing it all to stress or a busy schedule, check one simple number on your blood report: your Vitamin D level.
If your blood report shows a low 25-OH Vitamin D value, you are far from alone — and the good news is that it is entirely correctable.
This article explains what your Vitamin D test result means, why deficiency is so widespread in India, what symptoms to watch for, and how to treat it effectively.
What Is Vitamin D and Why Does It Matter?
Vitamin D is a fat-soluble vitamin that functions more like a hormone than a nutrient. Almost every cell in the body has Vitamin D receptors, which tells you how fundamental it is to normal function.
Its most well-known role is regulating calcium and phosphorus absorption, which keeps bones strong and dense. But that is just the beginning.
Vitamin D also plays a critical role in immune function, muscle strength, mood regulation, insulin sensitivity, and cardiovascular health.
A deficiency, therefore, does not just affect your bones. It creates a ripple effect across multiple body systems — which is why a low Vitamin D result on a blood report deserves prompt attention, not just a note to eat more fish.
Why Is Vitamin D Deficiency So Common in India?
India receives abundant sunlight year-round. So why is Vitamin D deficiency a national epidemic?
Studies estimate that 70-90% of urban Indians and 40-80% of rural Indians have deficient or insufficient levels. This is not unique to any age group — deficiency is widespread across children, working-age adults, and the elderly alike.
The answer lies not in how much sun India gets — but in how little of it most Indians actually absorb.
| The Indian paradox A country with 300+ sunny days a year has one of the highest rates of Vitamin D deficiency in the world. Lifestyle, skin type, pollution, and diet all contribute — often simultaneously. |
How Does the Body Make Vitamin D?
Think of Vitamin D production as a three-step relay race:
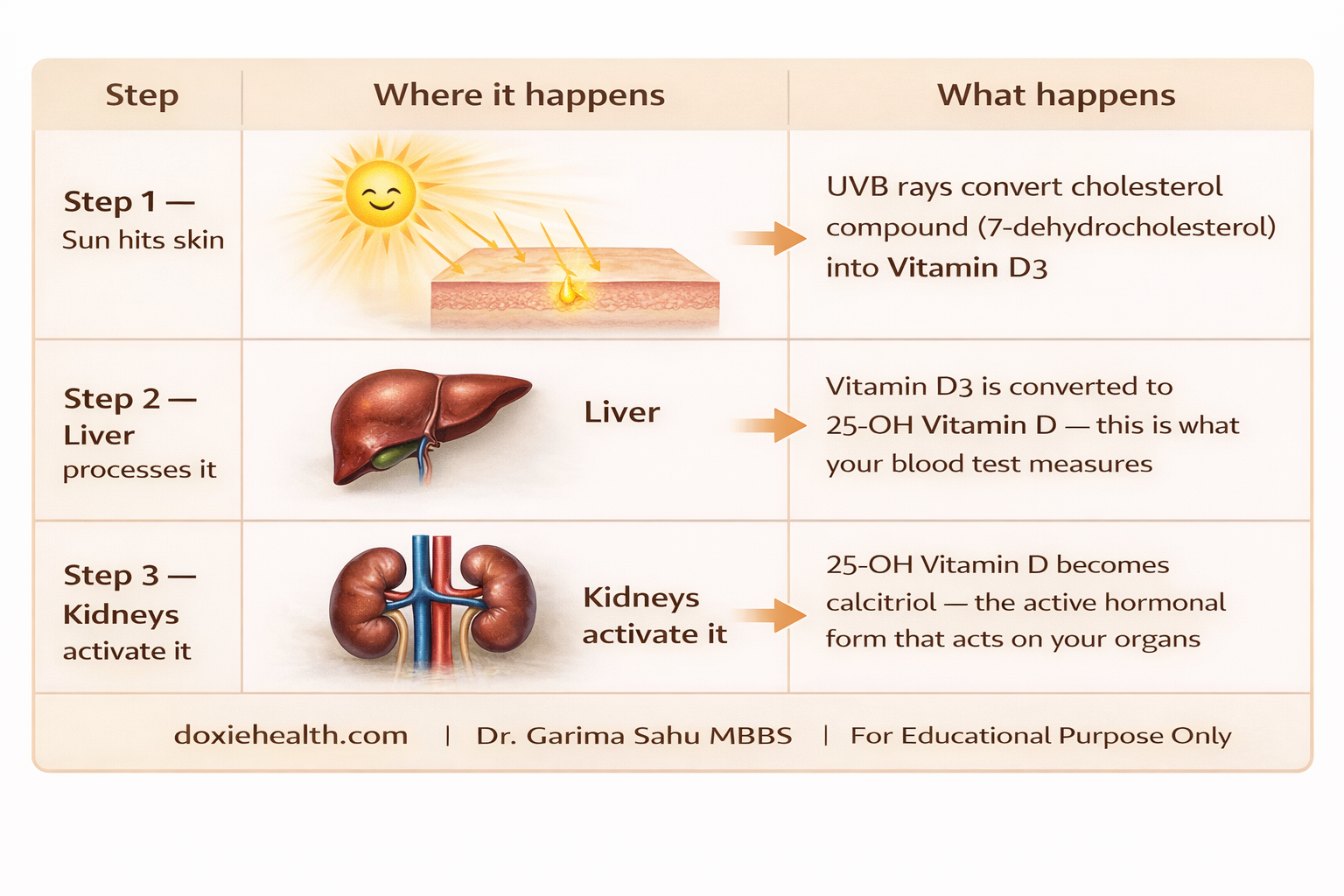
A problem at any step — too little sun, liver disease, or kidney dysfunction — can result in deficiency even if you are eating well and spending time outdoors.
| What the blood test measures: Step 2 Your test reports measure 25-OH Vitamin D (the liver output) — not the final activated form. This is intentional: 25-OH Vitamin D has a longer half-life in the blood and gives the most accurate picture of your body’s Vitamin D stores. |
What Causes Vitamin D Deficiency in India?
It is rarely one factor. For most Indians, several causes stack on top of each other simultaneously:

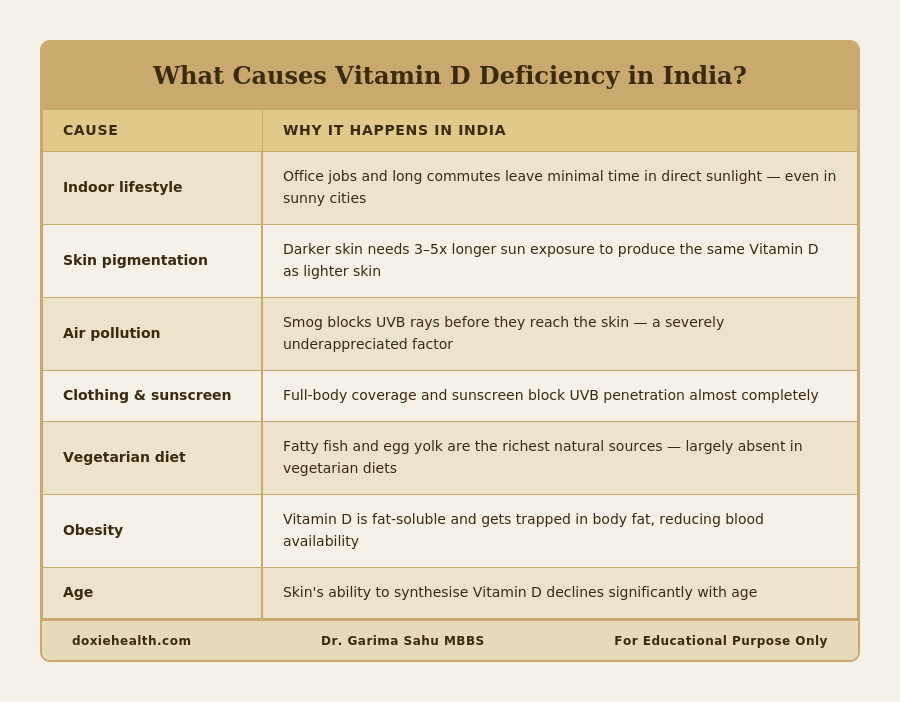
| The compounding effect. An office worker in Delhi with dark skin, who commutes by car, applies sunscreen daily, eats a vegetarian diet, and lives in a smoggy neighbourhood, is facing every single risk factor simultaneously. This describes millions of Indians. |
Symptoms of Vitamin D Deficiency
Vitamin D deficiency is often silent in early stages. When symptoms appear, they are non-specific and are frequently attributed to stress or overwork, which is why they are so commonly missed.

Common symptoms
- Persistent fatigue and low energy despite adequate sleep
- Diffuse bone pain — particularly in the lower back, hips, and legs
- Muscle weakness and generalised body aches
- Frequent infections — colds, flu, or prolonged recovery from illness
- Low mood, irritability, or mild depression
- Hair loss — linked to Vitamin D receptor activity in hair follicles
In severe or prolonged deficiency
- Rickets in children — softening and deformity of bones
- Osteomalacia in adults — bone softening causing fractures with minimal trauma
- Proximal myopathy — difficulty climbing stairs or rising from a chair due to muscle weakness
Conditions independently associated with low Vitamin D
Low Vitamin D is independently linked to lower HDL and higher triglycerides — two key components of an abnormal lipid profile. If your Vitamin D is low and your cholesterol report is also abnormal, the two are likely connected. Read our detailed guide on understanding and managing your lipid profile: https://doxiehealth.com/lipid-profile-explained/
Vitamin D also plays a role in red blood cell production. Deficiency can worsen existing iron deficiency anaemia, which is why doctors often check both together when fatigue and low energy are the presenting complaints. To understand how anaemia shows up on your blood report, read: https://doxiehealth.com/iron-deficiency-anemia/
| Condition | Connection |
| Hypothyroidism | Low Vitamin D worsens thyroid autoimmunity (Hashimoto’s) |
| Dyslipidaemia | Low Vitamin D linked to lower HDL and higher triglycerides |
| Anaemia | Vitamin D plays a role in red blood cell production — deficiency can worsen iron deficiency anaemia |
| Insulin resistance / Type 2 diabetes | Vitamin D receptors are present in pancreatic beta cells — deficiency impairs insulin secretion |
| Autoimmune conditions | Multiple sclerosis, rheumatoid arthritis, and psoriasis are all associated with low Vitamin D |
Understanding Your Vitamin D Test Report
Your Vitamin D test measures 25-hydroxyvitamin D (25-OH Vitamin D) in the blood. This is the correct test to order — not 1,25-dihydroxyvitamin D, which does not accurately reflect body stores.
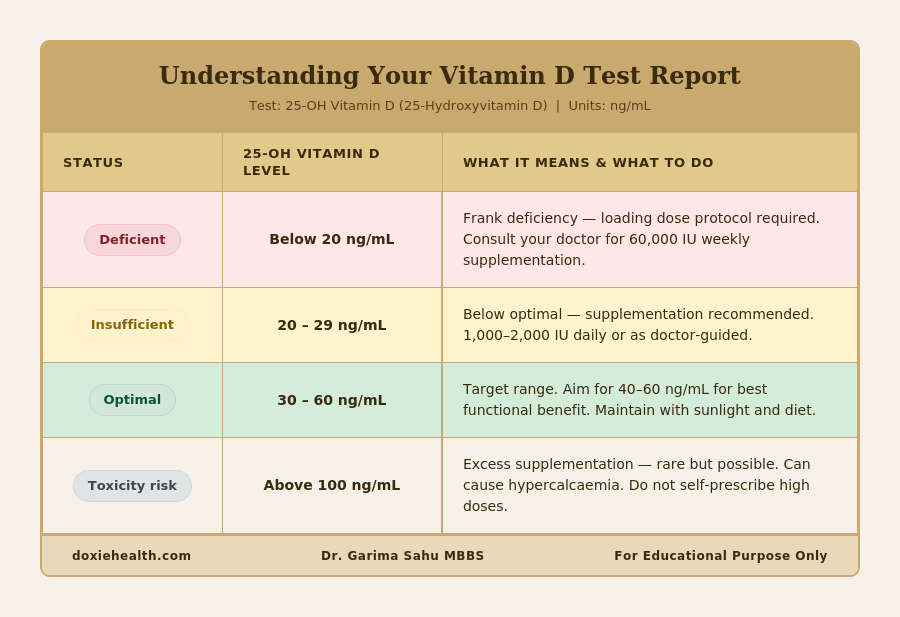
Vitamin D test result ranges showing deficient, insufficient, optimal and toxicity levels. Image: DoxieHealth| Important: Many Indian labs list the normal range as 20-100 ng/mL. Most current guidelines consider below 30 ng/mL as insufficient. Aim for 40-60 ng/mL as your functional optimal — not just ‘not deficient’. A result of 18 ng/mL is not borderline — it is deficient and warrants treatment. |
Treatment — How to Correct Vitamin D Deficiency

1. Sunlight — the primary source
15-20 minutes of direct midday sun (10 am-2 pm) on arms, legs, and face — without sunscreen — on most days of the week.
Darker skin tones may need 30-40 minutes for the same output.
Glass windows block UVB entirely, so sitting near a sunny window does not count.
2. Dietary sources
| Food source | Vitamin D content | Suitable for |
| Fatty fish (salmon, mackerel, sardines) | 400-600 IU per 100g | Non-vegetarian |
| Egg yolk | ~40 IU per yolk | Both |
| Fortified milk | 100 IU per cup | Both |
| Fortified cereals | 40-100 IU per serving | Both |
| UV-exposed mushrooms | Up to 400 IU per 100g | Vegetarian |
| Cod liver oil | 450 IU per tsp | Non-vegetarian |
| Note for vegetarians: Natural food sources of Vitamin D are extremely limited in a vegetarian diet. UV-exposed mushrooms are the only significant plant-based source. Supplementation is practically essential for most Indian vegetarians with a deficiency. |
3. Supplementation
| Deficiency level | Typical approach |
| Deficient (below 20 ng/mL) | 60,000 IU weekly for 8-12 weeks (loading dose), then maintenance |
| Insufficient (20-29 ng/mL) | 1,000-2,000 IU daily or 60,000 IU fortnightly |
| Maintenance (once optimal) | 1,000-2,000 IU daily |
| Important: Vitamin D3 (cholecalciferol) is preferred over D2 — more effective at raising and maintaining blood levels Always take with a fat-containing meal — absorption drops significantly on an empty stomach Recheck 25-OH Vitamin D after 3 months of supplementation to confirm correction |
Key Clinical Insights
- Vitamin D toxicity is rare but real. Levels above 100 ng/mL from excess supplementation can cause hypercalcaemia.
- This does not happen from sunlight — only from excessive long-term dosing. Do not self-prescribe above 2,000 IU daily without medical guidance.
- Magnesium is required to activate Vitamin D.
- If levels are not rising despite supplementation, magnesium deficiency may be the reason — it is a cofactor in the conversion pathway and is also commonly low in India.
- Vitamin D and thyroid: Low Vitamin D worsens Hashimoto’s thyroiditis. Correcting Vitamin D often supports better thyroid antibody control.
- Recheck before stopping supplementation. Symptoms improve before blood levels fully normalise. Always confirm the correction with a repeat test.
| Doctor’s Note In my clinical experience, Vitamin D deficiency is one of the most underdiagnosed conditions in India — not because tests are unavailable, but because the symptoms are so non-specific that both patients and doctors attribute them to stress or overwork. If you have persistent fatigue, bone pain, or frequent infections, ask for a 25-OH Vitamin D test. It is inexpensive, widely available, and entirely actionable. |
| When Should You Be Concerned? 25-OH Vitamin D below 20 ng/mL — frank deficiency requiring a loading dose protocol. Bone pain, muscle weakness, or difficulty walking alongside a low result. Levels not improving after 3 months of supplementation — rule out malabsorption. Known autoimmune condition, thyroid disorder, or diabetes — Vitamin D correction is part of comprehensive management. Pregnancy or planning pregnancy — Vitamin D deficiency has serious implications for foetal bone development. |
The Takeaway
Vitamin D deficiency is silent, widespread, and correctable. A simple blood test — 25-OH Vitamin D — tells you exactly where you stand. If your level is below 30 ng/mL, a combination of sensible sun exposure, dietary adjustments, and supplementation will reliably correct it within 3 months.
The key is to retest, confirm correction, and maintain optimal levels long-term — not just treat once and forget.
Questions to Ask Your Doctor
- My Vitamin D is low — do I need a loading dose or can I start with daily supplementation?
- Should I also check my calcium, magnesium, and parathyroid hormone levels?
- I am a vegetarian — what is the best supplement form and dose for me?
- How long should I supplement before retesting?
- Do my thyroid condition or cholesterol levels need to be reviewed alongside Vitamin D correction?
References
1. Holick MF. Vitamin D Deficiency. New England Journal of Medicine. 2007;357:266-281. Read here →
2. Ritu G, Gupta A. Vitamin D Deficiency in India: Prevalence, Causalities and Interventions. Nutrients. 2014;6(2):729-775. Read here →
3. Lips P. Vitamin D Physiology. Progress in Biophysics and Molecular Biology. 2006;92(1):4-8. Read here →
4. Pludowski P et al. Practical guidelines for supplementation of Vitamin D. Endokrynologia Polska. 2013;64(4):319-327. Read here →
5. Harrison’s Principles of Internal Medicine, 21st Edition. McGraw-Hill, 2022.



Leave a Reply